“Tiene que haber un cambio en Nicaragua”: reflexiones a seis años de la Rebelión de Abril
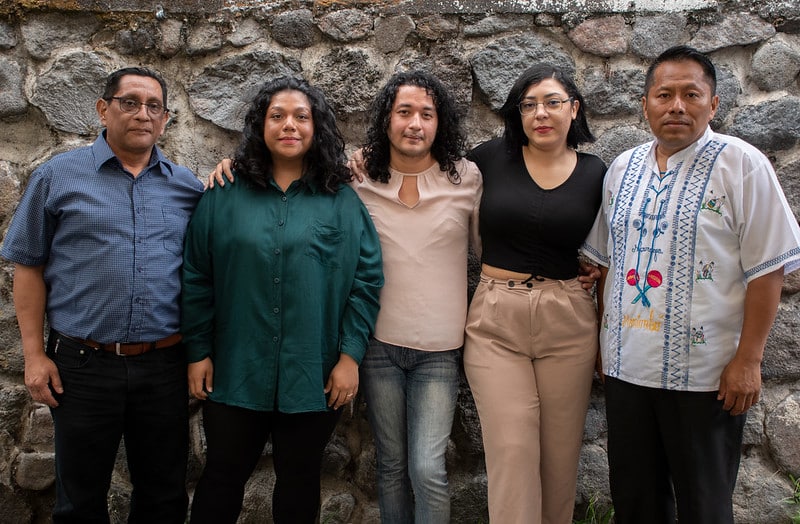
“No nos arrepentimos de nada”. Cinco nicaragüenses que participaron en la Rebelión de Abril exaltan el coraje de la ciudadanía frente a la dictadura

































